Do You Really Need a Liver Detox? A Pharmacist Explains What Works and What's Just Marketing

Last week, a patient told me she felt "toxic." Not in a dramatic way, just tired to her bones. She was juggling work, family, and a calendar full of refills. A few meds for blood pressure, something for sleep, and cancer medications that made food taste like metal. Then her feed served a parade of ads: liver drops, detox teas, "7-day cleanses," and a promise to feel brand new by Friday.
If you're in that spot, it's easy to wonder if a Liver Detox is the missing piece. The marketing sounds caring, almost clinical. Yet the liver isn't a clogged drain that needs a weekly flush. It's a working organ that's already cleaning, sorting, and shipping waste all day.
From a pharmacist's point of view, this post breaks down what your liver actually does, what detox marketing gets wrong, what habits and products have real signal for Liver Health, and when it's time to call your clinician. Consider this a clear, calm checkpoint in the style of the Waldrugmart Health Guide.
https://www.youtube.com/watch?v=UYNOjPbv2nw
What your liver really does all day (and why it's already a detox machine)
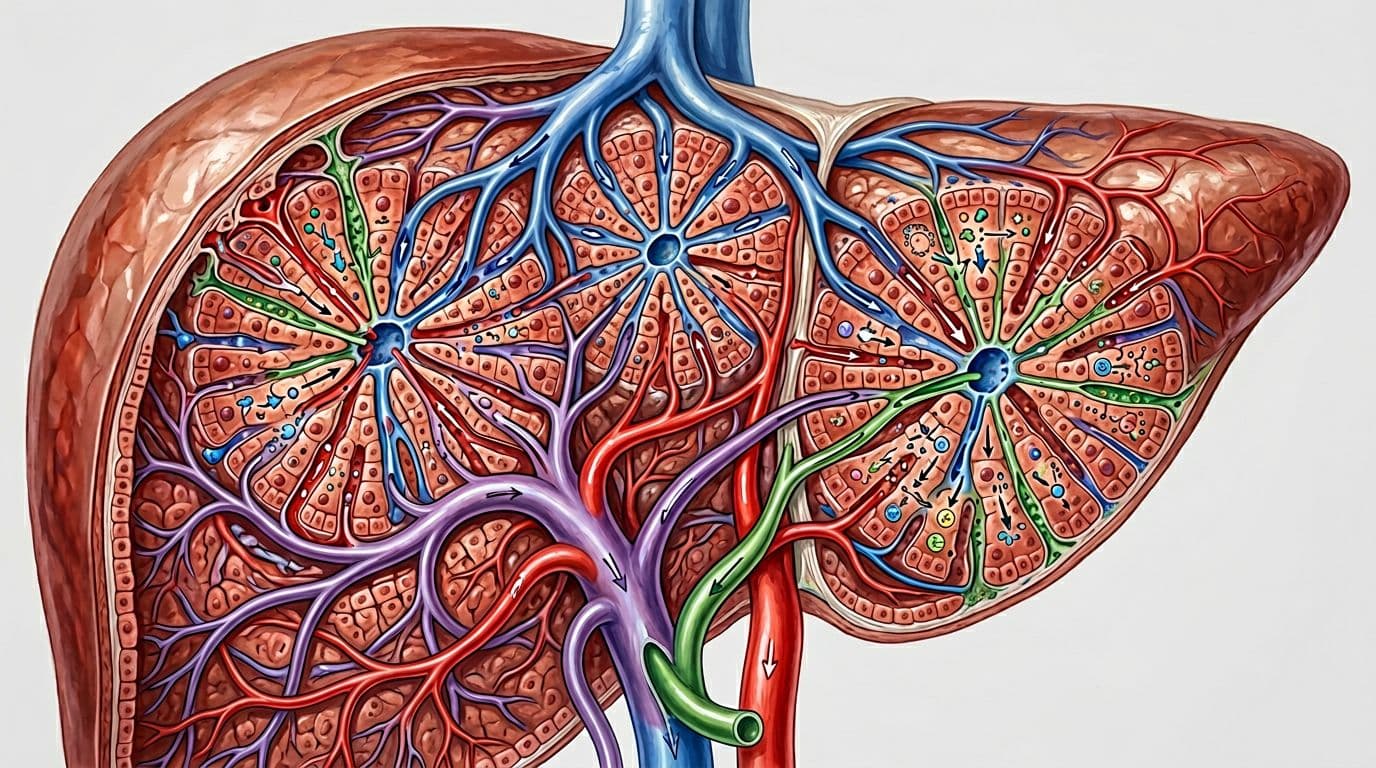 An anatomical view of the liver's internal "plumbing" and processing pathways, created with AI.
An anatomical view of the liver's internal "plumbing" and processing pathways, created with AI.
Picture your liver like a busy shipping warehouse. Blood flows in carrying nutrients, hormones, and medication leftovers. The liver checks the "labels," changes what needs changing, and sends packages out through bile or back to the blood for the kidneys to finish.
Here's what it handles, quietly, every day:
- It filters blood coming from the gut, which matters after meals and after alcohol.
- It processes many medications, which is why some drugs can't be mixed.
- It makes bile, a fluid that helps you digest fats and remove certain waste.
- It stores energy as glycogen, then releases it when you're between meals.
- It runs chemical pathways that turn compounds into forms your body can remove.
Detox marketing often frames the goal as a quick purge. In real life, the goal is steady support: enough protein, enough sleep, safe medication use, and fewer daily hits (like alcohol or excess sugar). That's not as flashy as a three-day cleanse, but it's how bodies improve.
One hard safety point belongs here: don't stop prescribed medications for a cleanse. If a product tells you to "pause meds so the detox can work," treat that as a red flag, not a health plan. If you're worried your medicines affect your liver, ask the clinician who prescribed them, or ask a pharmacist to review them.
For a plain-language myth check, Johns Hopkins has a helpful overview on liver detox fact versus fiction.
Phase 1 and Phase 2 detox, explained like you're reading a label
Your liver's detox work gets described as Phase 1 and Phase 2. You don't need a biochem degree to understand the big idea.
Phase 1 is the breakdown step. Enzymes change a substance into a new form. Sometimes that new form is more reactive for a short time, kind of like breaking a big box into smaller pieces.
Phase 2 is the pack-and-ship step. The liver attaches helper molecules (think: a shipping label) so the body can move the substance out through bile or urine.
A simple analogy helps: it's a two-step factory line. Step one cuts materials. Step two boxes them up and sends them out. If you push the first step faster but don't support the second step, you can feel worse, not better.
That "detox headache" some people get after a cleanse doesn't prove toxins are leaving. It often lines up with caffeine withdrawal, low calories, dehydration, or laxative effects. Nausea can happen for the same reasons.
If a product makes you feel shaky, dizzy, or dehydrated, that's not your body "resetting." That's a side effect.
When the liver struggles, it's usually not from "toxins," it's from daily wear and tear
Most real liver problems aren't mysterious. They come from stressors we recognize, day after day.
Alcohol is a clear one. So is fatty liver disease, now often tied to weight, insulin resistance, and high triglycerides. You'll still hear the older, simple stat that fatty liver affects about 1 in 4 adults. Some more recent U.S. analyses suggest it may be higher, which fits what clinicians are seeing in practice.
Viral hepatitis remains important, especially if someone never got screened. Medication side effects can matter too, including interactions, high doses, or stacking multiple products that stress the liver.
Sleep and stress don't "clog" the liver, but they change hormones, appetite, and inflammation. Over time, that can nudge weight and blood sugar in the wrong direction, which then nudges the liver.
If you have diagnosed liver disease, a "cleanse" is not the first tool. Targeted treatment is. For example, clinicians may prescribe ursodeoxycholic acid for specific bile-related conditions. If you're ever prescribed it, keep refills consistent and follow your lab schedule (one reference point is this product page for Generic Ursodiol tablets).
Why liver detox products sell so well (and how to spot the marketing tricks)
 A patient and pharmacist reviewing supplement choices and safety, created with AI.
A patient and pharmacist reviewing supplement choices and safety, created with AI.
Detox products sell because they tell a simple story: you feel bad because you're "full of toxins," and you can fix it fast. That story feels comforting when you're tired, bloated, or on a long list of meds.
The problem is evidence. In generally healthy people, most detox teas, drops, and multi-ingredient "liver cleanse" kits don't have strong proof that they improve liver function. Some can even cause harm, especially in higher doses or with long use.
Detox marketing also borrows the look of medicine. You'll see words like "clinically proven" without clear references, or "doctor-formulated" without a named clinician and their credentials. Before-and-after photos often reflect less food, less salt, and water loss, not a changed liver.
If you want one fast way to evaluate a claim, ask: What measurable outcome should change? Liver enzymes on labs? Symptoms? Imaging? If the only outcome is "feel lighter," the product is selling a feeling, not liver function.
Here's a quick reality check on common claims:
| Marketing claim | What it often means in real life | What to ask instead |
|---|---|---|
| "Flush toxins fast" | Laxative or diuretic effect, less food intake | "Does it improve labs or diagnosis outcomes?" |
| "Reset your liver" | A catchy phrase, no medical definition | "Reset from what, and how is it measured?" |
| "Melt liver fat" | Short-term weight drop, mostly water | "Is there evidence for fatty liver improvement?" |
| "Remove heavy metals" | Big promise, little proof for OTC blends | "Was contamination tested and documented?" |
Independent groups have been calling out detox claims for years. Sense about Science compiled evidence gaps in their detox debunking project, and the theme hasn't changed much.
A label "gut check" helps too. Look for proprietary blends (unknown doses), mega-doses of single vitamins, stimulant laxatives, diuretics, and vague "detox complexes." Also notice what's missing: lot numbers, clear dosing, and third-party testing.
Red-flag claims: "flush toxins fast", "reset your liver", and "microplastics cleanse"
"Flush toxins fast" is shaky because your body removes waste at the pace your liver, gut, and kidneys can handle. Speeding things up with diarrhea doesn't upgrade detox pathways. It just drains fluid.
"Reset your liver" sounds medical, but it's not. The liver can heal in some settings, yes, but it heals with time and by removing the stressor (like alcohol). A reset isn't a weekend event.
Then there's the newer trend, especially loud in March 2026: microplastics detox claims. The science on microplastics is still developing, and researchers are studying where particles end up and what they do. However, "detox kits" claiming to pull microplastics out of organs are way ahead of evidence. For most people, the best-known steps are boring but real: reduce exposure where you can, keep fiber intake solid, and let normal elimination do its job.
That "lighter" feeling after a cleanse often comes from less food volume, less salt, water loss, or a laxative effect. None of those automatically equal better Liver Health.
For another grounded overview of claims versus facts, Healthgrades summarizes myths and facts about detoxifying the liver.
Detox teas and extreme cleanses can backfire, especially if you take prescriptions
The biggest detox risk I see is simple: people treat supplements like food, then mix them with complex medication regimens.
Detox teas can cause dehydration and electrolyte swings. That matters if you're on diuretics, heart meds, or blood pressure medications. Laxative-heavy cleanses can also change how fast pills move through your gut, which can change absorption.
Interactions are another issue. Some herbs can affect liver enzymes that process medications. Others raise bleeding risk or change blood sugar. People who should be extra careful include anyone taking blood thinners, diabetes meds, seizure meds, transplant meds, cancer medications, or multiple prescriptions.
If you order refills through an Online Pharmacy, the safest process includes prescription verification and an option to ask questions before you add supplements. A reliable Online chemist workflow should still treat interactions seriously, even when the product looks "natural."
A practical tip: if you're considering a detox product, write down everything you take (prescriptions, OTC meds, and supplements). Then ask a pharmacist, "What's the interaction risk here?" That one question prevents a lot of trouble.
What actually supports liver health (and what a pharmacist would pick first)
 Everyday foods linked to antioxidant support and healthy metabolism, created with AI.
Everyday foods linked to antioxidant support and healthy metabolism, created with AI.
If your liver could talk, it probably wouldn't ask for a cleanse. It would ask for fewer hits and more consistency. That's good news because it means your next step can be simple, not expensive.
Start with the basics that move the needle the most:
- Drink less alcohol, or stop if you have liver disease.
- Aim for steady weight loss if you need it, even 5 to 10% can matter.
- Build meals around whole foods, especially fiber and protein.
- Move most days, even if it's just walking after dinner.
- Protect sleep, because poor sleep pushes cravings and insulin resistance.
Food doesn't "detox" you, but it supports the pathways your liver already runs. Cruciferous vegetables (like broccoli) provide compounds your body uses in processing. Garlic and onions bring sulfur compounds that fit into normal detox chemistry. Beets add nitrates and antioxidants. Eggs provide amino acids your liver uses for packaging and shipping steps. Vitamin C-rich foods support antioxidant systems.
Hydration is the unglamorous helper here. Water keeps blood volume steady and supports normal kidney elimination, which works alongside the liver.

Photo by Pixabay
A "start here this week" plan should feel doable on a tired Tuesday:
- Pick three alcohol-free days (or none at all if advised).
- Add one high-fiber food daily (beans, berries, oats, or veggies).
- Walk 10 minutes after one meal each day.
- Set a fixed "screens off" time, even 20 minutes earlier.
- Don't add a new supplement without an interaction check.
In some cases, real liver disease needs real medication, not a cleanse. Hepatitis C, for example, can require antiviral therapy under clinician guidance. If you're on treatment, consistency matters (one reference is Sofosbuvir hepatitis C treatment, which should always be used only with a valid prescription and monitoring).
Daily habits that help more than any cleanse
Small habits beat big detox promises because they work with biology, not against it.
Alcohol deserves a clear mention because it's directly processed in the liver. If you drink, keep it moderate, and be honest with your clinician about how much. Next, focus on blood sugar and weight, because fatty liver often tracks with insulin resistance.
Fiber is a quiet hero. It supports regular bowel movements, which is one of the body's main waste exits. It also feeds gut bacteria that may influence inflammation in the gut-liver axis.
Movement helps in two ways: it improves insulin sensitivity, and it reduces liver fat over time. You don't need a gym membership for that. Walking, light resistance bands, or short home routines count.
Sleep is the habit people dismiss first, yet it shapes appetite hormones and stress signaling. If you can't sleep due to symptoms or meds, bring it up. Sometimes a dosing change, timing shift, or safer sleep plan helps more than any supplement.
Finally, don't forget medication basics. Take acetaminophen only as directed, avoid doubling cold products that contain it, and don't stack "liver support" pills without a plan.
Supplements: what has some evidence, what to avoid, and how to use them safely
Supplements sit in a tricky space. Some have promising data for specific contexts, but few are magic, and "natural" doesn't mean safe.
A few ingredients have a better signal than most detox blends:
NAC (N-acetylcysteine) supports pathways that help build glutathione, one of the body's key antioxidants. Clinicians also use NAC as a medication in acetaminophen overdose. That doesn't mean everyone should take it daily, but it explains why it's taken seriously in medical settings.
Glycine is an amino acid involved in glutathione support and other metabolic functions. Early research suggests possible benefits in inflammation pathways, although dosing and real-world impact vary.
Glutathione-support nutrient blends may raise glutathione markers in some human studies, but product quality matters a lot. Also, raising a marker isn't the same as treating a disease.
What to avoid: proprietary "detox stacks" with long ingredient lists, stimulant laxatives dressed up as "cleansing," and megadose blends that don't match any clear need. Be cautious with any product that encourages frequent use or escalating doses.
Safer buying tends to look boring: single-ingredient products, clear dosing, and third-party testing when possible. Most importantly, avoid starting several new products at once. If something causes a side effect, you won't know what did it.
Milk thistle (silymarin) is commonly marketed for liver support, and some people ask about it first. If you consider it, choose a reputable product and still check interactions (one example listing is 80% Silymarin liver support capsules).
A final safety point: if you manage multiple medications, keep refills consistent and keep one up-to-date med list. Interaction checks are part of good pharmacy care, whether you fill locally or through an Online Pharmacy that verifies prescriptions and supports ongoing refills.
For a look at how popular "liver cleansing" products get analyzed, the American College of Gastroenterology published an abstract on liver cleansing imposters.
Conclusion
Your liver already detoxes. It doesn't wait for a tea, a dropper, or a seven-day reset. Most Liver Detox products sell a feeling, not a measurable improvement. Real Liver Health looks less dramatic and more steady: fewer stressors (especially alcohol), better sleep, more fiber, regular movement, and careful medication use. Supplements like NAC or glycine may help in some situations, but they're not risk-free, especially when you're on multiple prescriptions.
Call a clinician right away if you notice yellow skin or eyes, dark urine, pale stools, severe belly pain, swelling, confusion, vomiting blood, sudden bruising, or new medication side effects. If you're thinking about a detox product while taking prescription medications or cancer medications, ask a pharmacist first. Clear, practical safety advice beats marketing every time, and that's the standard worth keeping.
